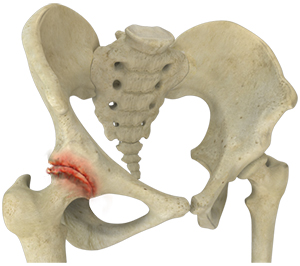
What is Osteoarthritis of the Hip?
Osteoarthritis, also called degenerative joint disease, is the most common form of arthritis. It occurs most often in the elderly. This disease affects the tissue covering the ends of bones in a joint called cartilage. In osteoarthritis, the cartilage becomes damaged and worn-out, causing pain, swelling, stiffness and restricted movement in the affected joint. Although osteoarthritis may affect various joints including the hips, knees, hands, and spine, the hip joint is most commonly affected. Rarely, the disease may affect the shoulders, wrists, and feet.
What are the Causes of Osteoarthritis of the Hip?
Advanced age is one of the most common reasons for osteoarthritis of the hip. You may also develop osteoarthritis in the following cases:
- Previous hip injury or fracture
- Family history of osteoarthritis
- Suffer from hip diseases such as avascular necrosis and other congenital or developmental hip diseases
What are the Symptoms of Osteoarthritis of the Hip?
You will experience severe pain that is confined to the hip and thighs, morning stiffness and limited range of motion.
How is Osteoarthritis of the Hip Diagnosed?
Based on your symptoms, your doctor will perform a physical examination, X-rays and other scans, and some blood tests to rule out the other conditions that may cause similar symptoms.
How is Osteoarthritis of the Hip Treated?
There are several treatments and lifestyle modifications that can help you ease your pain and symptoms.
- Medications: Pain-relieving medications such as NSAIDs and opioids may be prescribed. Topical medications such as ointments can be applied over the skin to relieve pain. If the pain is very severe, corticosteroid injection can be administered directly into the affected joint to ease the pain.
- Other treatments: Your physiotherapist will teach you exercises to keep your joints flexible and improve muscle strength. Heat/cold therapy that involves applying heat or cold packs to the joints provides temporary pain relief. Lifestyle modifications are encouraged to control your weight and avoid extra stress on the weight-bearing joints.
- Surgery: Hip joint replacement surgery is considered as an option when the pain is so severe that it affects your ability to carry out normal activities.
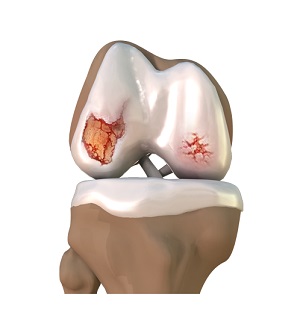
What is Knee Osteoarthritis?
Knee osteoarthritis (OA) is a degenerative joint disease that occurs when the cartilage in the knee joint gradually wears away. Cartilage is a smooth, slippery tissue that cushions the ends of bones and helps the joint move smoothly. As it deteriorates, the bones may begin to rub against each other, leading to pain, swelling, stiffness, and reduced mobility. Knee osteoarthritis primarily affects older adults but can occur in younger individuals as well.
What are the Causes of Knee Osteoarthritis?
Common causes and risk factors of knee osteoarthritis include:
- Aging: Most common in people over 50.
- Joint injury or overuse: Repetitive stress or trauma can accelerate wear.
- Obesity: Extra weight adds stress to the knee joint.
- Genetics: Family history can increase risk.
- Other joint conditions: Such as rheumatoid arthritis or gout.
- Joint malalignment: Such as bowlegs (varus) or knock knees (valgus) can increase risk.
What are the Signs and Symptoms of Knee Osteoarthritis?
Common symptoms of knee osteoarthritis include:
- Pain: Worsens with activity and improves with rest.
- Stiffness: Especially after resting or in the morning.
- Swelling: Due to inflammation or fluid buildup.
- Limited movement: Difficulty bending or straightening the knee.
- Grinding or clicking sounds: Felt or heard during movement.
- Weakness or instability: The knee may feel like it could give out.
How is Knee Osteoarthritis Diagnosed?
The diagnosis of knee osteoarthritis is typically based on a combination of clinical evaluation and imaging studies. A physician will begin with a detailed medical history and physical examination, assessing symptoms such as joint pain, stiffness, swelling, and reduced mobility. During the physical exam, the doctor may check for tenderness, crepitus (a grinding sound), and joint instability. Imaging studies, especially X-rays, are commonly used to confirm the diagnosis by revealing characteristic changes like joint space narrowing, bone spurs (osteophytes), and changes in bone shape. In some cases, an MRI may be ordered to evaluate soft tissue structures such as cartilage and ligaments, particularly if the diagnosis is unclear or other joint issues are suspected. Laboratory tests may also be conducted to rule out other conditions like rheumatoid arthritis or gout.
How is Knee Osteoarthritis Treated?
Treatment for knee osteoarthritis aims to reduce pain, improve joint function, and slow the progression of the disease. Non-surgical options are typically tried first and include lifestyle modifications such as weight loss and regular low-impact exercises to reduce stress on the knee. Medications like acetaminophen or non-steroidal anti-inflammatory drugs (NSAIDs) can help relieve pain and inflammation, while physical therapy focuses on strengthening the muscles around the knee and improving flexibility. In some cases, patients may benefit from corticosteroid or hyaluronic acid injections to reduce inflammation and enhance joint lubrication. Emerging therapies like platelet-rich plasma (PRP) or stem cell injections are also being explored. Supportive devices such as knee braces or orthotics can help offload pressure from the affected area. When conservative treatments are no longer effective and symptoms become severe, surgical options such as arthroscopy, osteotomy, or partial or total knee replacement may be considered to restore mobility and reduce pain.
If you would like guidance on the most appropriate treatment, please call to schedule an appointment or click to request an appointment online.

